
Lifestyle risks for chronic disease among Australian adolescents: a cross-sectional survey
Physical inactivity, poor diet, alcohol use, smoking, poor sleep, and excessive recreational screen time are lifestyle risk factors that emerge during adolescence, continue into adulthood, and often occur together. They are linked with obesity and mental health problems in the short term, and with increased risk of chronic disease in adulthood.
Research, led by Dr Katrina Champion and Associate Professor Cath Chapman at the University of Sydney's Matilda Centre, investigates the prevalence and socio-demographic correlates of these major lifestyle risk factors in a large sample of Australian adolescents. The findings have been published as a research letter in the Medical Journal of Australia.
The authors analysed baseline data from more than 6,600 young Australians who participated in the Health4Life Study. The Health4Life Study is a cluster randomised controlled trial of an e-health intervention in 71 independent, catholic, and government secondary schools from New South Wales, Western Australia, and Queensland.
6,640 students aged 11‒14 years (mean, 12.7 years; standard deviation, 0.5 years); 3,311 were boys (50.6%) completed an online self-report survey assessing:
- moderate-to-vigorous physical activity
- sedentary recreational screen time
- sleep duration
- diet (including sugar-sweetened beverages, fruit and vegetables discretionary food items)
- alcohol
- tobacco use.
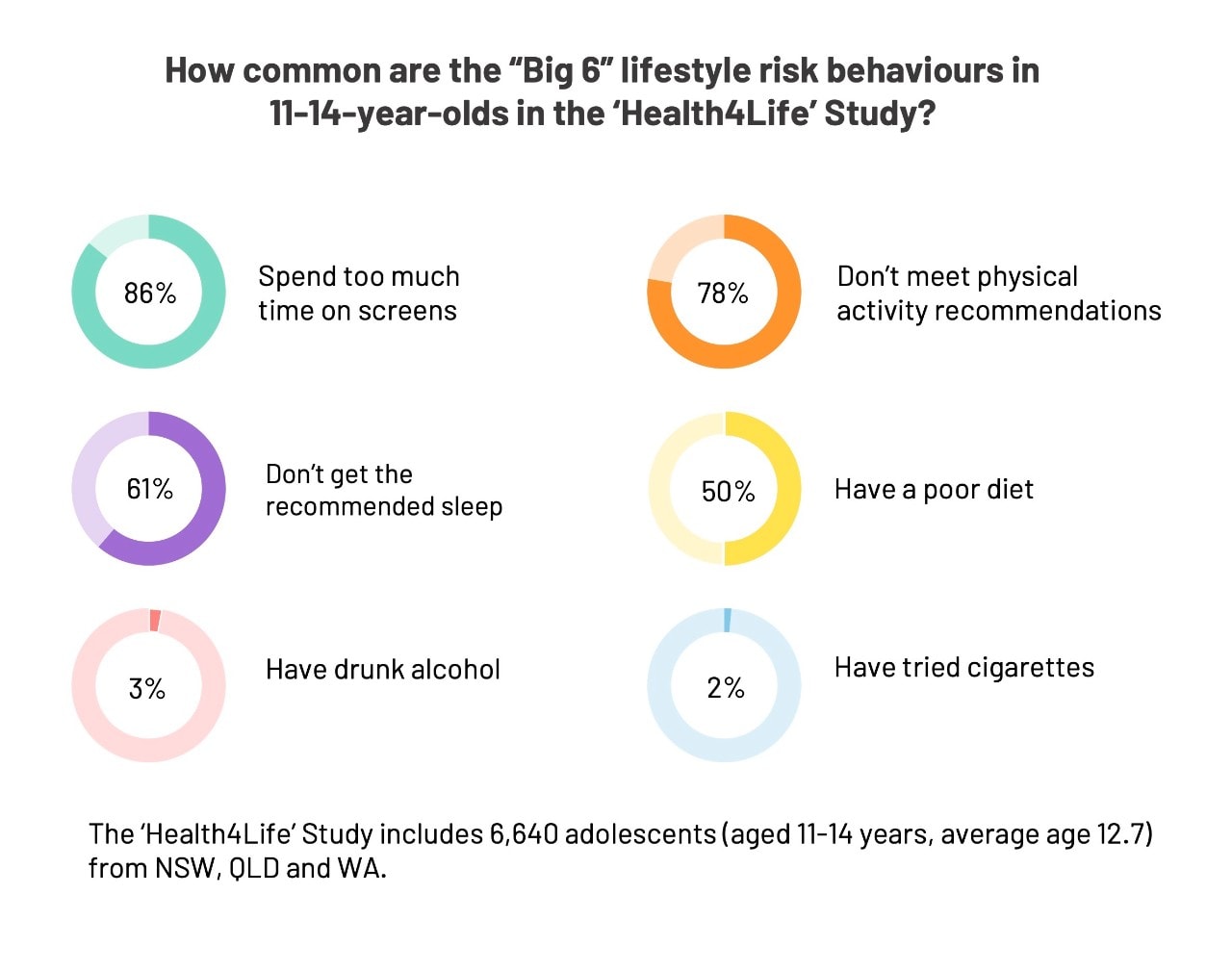
Screen time (85.9%), physical inactivity (77.7%) and poor sleep (61.3%) were prevalent, and most students reported several risk behaviours (three or more, 62.7%; four or more, 25.6%).

Dr Katrina Champion
"It's concerning that a large proportion of our sample were engaging in multiple risk behaviours at once, as we know that this can increase the risk of health problems in adolescence and in later life," says Dr Champion.
Risk behaviours varied by socio-demographic factors, particularly gender. The findings highlight the need for preventive public health strategies targeting adolescent lifestyle factors that take gender, socio-economic status, and remoteness into account.

Associate Professor Cath Chapman
So, how can we address these risk factors and promote healthy lifestyle behaviours in adolescence and beyond? "Screening by general practitioners for the six major risk factors and identifying young people with multiple risk behaviours could facilitate early intervention," explains Associate Professor Cath Chapman. The authors also suggest that brief interventions delivered in primary care or school settings may be beneficial.
Acknowledgements
The Health4Life study is funded by the Paul Ramsay Foundation, and by the National Health and Medical Research Council through fellowships (Katrina Champion, APP1120641; Maree Teesson, APP1078407; Nicola Newton, APP1166377) and the Centre of Research Excellence in the Prevention and Early Intervention in Mental Illness and Substance Use (PREMISE; APP11349009). We thank the research assistants who collected data for the Health4Life study: Bridie Osman, Karrah McCann, Rhiannon Ellem, Jesse Whife, and Courtney Stewart. We also acknowledge the students and teachers at the participating schools.
