Research unlocks biomechanic mystery behind deadly blood clots
The findings take researchers one step closer to developing new anti-thrombotic drugs without the serious side effects that cause fatal bleeding.
While coagulation - the activation of platelets clumping together - is key to stopping blood loss from a cut or wound, overactivation can lead to deadly blood clots, heart attack or stroke.
Researchers have used a microfluidic channel, mimicking the narrowing of vessels that cause blood clots, to observe the activation of platelets at the single-molecular level.
Published in the prestigious journal Nature Materials, the researchers demonstrated blood flow disturbance could lead to previously unrecognised intermediate activation of integrin, an adhesion receptor that mediates platelet aggregation to form a clot. Integrin is a mechanosensory protein that platelets use to sense mechanical force generated by dynamic blood flow.
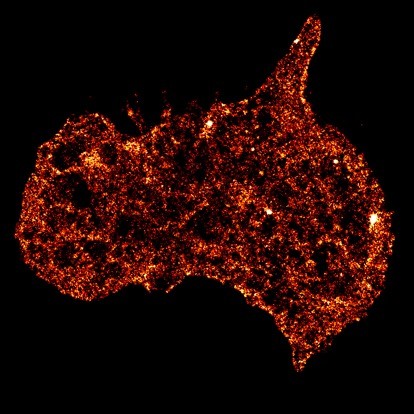
An activated human platelet – a blood clotting cell that plays a crucial role in preventing bleeding or causing the cardiovascular diseases such as heart attack and stroke.
Image credit: Lining Arnold Ju (University of Sydney) and Qian Su (University of Technology Sydney).
“Integrins basically facilitate how cells bind to and respond to their mechanical environment,” said Dr Arnold Lining Ju, co-lead author from the University of Sydney’s School of Aerospace, Mechanical and Mechatronic Engineering (AMME), Heart Research Institute (HRI) and Charles Perkins Centre (CPC).
“They allow cells to cling to each other, and are great communicators, transmitting bi-directional signals to activate the binding function; and outside-in, allowing the cell to sense and react to the extracellular environment. The integrin can instruct the platelet cells’ clotting behaviours.”
Dr Ju, an Australian Research Council DECRA Fellow in Biomedical Engineering at AMME and HRI, worked with a team of international researchers to develop a single-molecule biomechanical nanotool called “dual biomembrance force probe (BFP)” to observe how platelets harness mechanical force in blood flow to exert adhesive clotting functions.
Our finding may also offer help to diabetic patients since diabetic platelets are more prone resistant to conventional anti-clotting drugs.
The researchers say the finding – that biomechanical thrombus growth is mainly mediated by an intermediate state triggered by a unique integrin biomechanical activation pathway – has the potential to guide the development of new anti-thrombotic strategies. This could benefit many of the 55,000 Australians who suffer a heart attack each year - one every 10 minutes.
“Our finding may also offer help to diabetic patients since diabetic platelets are more resistant to conventional anti-clotting drugs,” said Dr Ju. "Targeting biomechanical pathways may also have the advantage of preventing deadly clots without bleeding side effects.
What the findings mean for current treatments
Dr Ju’s research also provides a new explanation for the poor efficacy of conventional antiplatelet drugs in the treatment of thrombotic cardiovascular diseases. Although these drugs inhibit the biochemical activation of platelets, they may not block the platelet biomechanical signaling pathways.
“Anti-platelet drugs such as Aspirin, Clopidogrel and Ticagrelor are commonly used for the treatment of thrombotic diseases. However, these drugs have serious side effects that cause fatal bleeding,” said Dr Ju.
“For a long time, studies in the field of thrombosis have attempted to understand the mechanism of platelet activation at the cellular and molecular levels, and hope to provide ideas for the development of new antithrombotic drugs with strong efficacy and few side effects.”
Senior Fellow at HRI Yuping Yuan said, “Since diabetes represents the biggest threat to the Australian health system, this discovery sheds light on protecting vulnerable diabetic individuals from heart diseases.”
The "mechanically driven platelet activation" phenomenon found in the study explains why platelets can aggregate and accumulate by mechanical stimulation of high-speed turbulence alone, leading to blockage of a blood vessel.
Therefore, this research provides new ideas for the development of novel and highly effective antithrombotic drugs with no serious bleeding side effects.
The paper, An integrin αIIbβ3 intermediate affinity state mediates biomechanical platelet aggregation, was published in Nature Materials.
Professor Shaun Jackson from HRI and CPC is a co-senior author on the research. Visiting scientists to the University of Sydney include Professor Cheng Zhu (co-senior author) from the Wallace H. Coulter Department of Biomedical Engineering at Georgia Tech and Emory University, Dr Yunfeng Chen (co-lead author) from the Scripps Institute, Prof Dayong Jin and Dr Qian Peter Su (co-authors) from University of Technology, Sydney.
Other researchers on this multi-disciplinary project were:
- Fangyuan Zhou and, Jiexi Liao (graduate student researchers in the Zhu lab at Georgia Tech);
- Lingzhou Xue (Penn State University);
- Hang Lu (Petit Institute researcher, and professor in the School of Chemical & Biomolecular Engineering at Georgia Tech).
Dr Ju’s research was funded by a National Heart Foundation Postdoctoral Fellowship and Australian Research Council DECRA Fellowship.
