
The global complexities of oral health

Comparison of estimated global case numbers for selected noncommunicable diseases.
Dr Bradley Christian, an external contributor to the report, says, “The global burden of oral diseases and their associated inequalities are alarming and at a tipping point. Without immediate action the burden on individuals and communities could become unmanageable”.
The report emphasises the importance of the social and commercial determinants of health and the need for a common risk factor approach to addressing disease burden. It reveals opportunities and challenges in engaging stakeholders to accelerate progress towards universal coverage for oral health and provides country oral health profiles based on the most updated oral health indicators to enable evaluation and monitoring.
The WHO are in the final stages of two more significant projects: the Global Oral Health Action Plan and accompanying Monitoring Framework, where a key strategic action is the integration of oral health into primary health care with a proposed target of 80% of countries achieving this by 2030. In collaboration with the WHO, Dr Christian is leading a systematic review, Effective strategies to integrate oral health into primary care, which will enable countries to translate the action plan into practice.
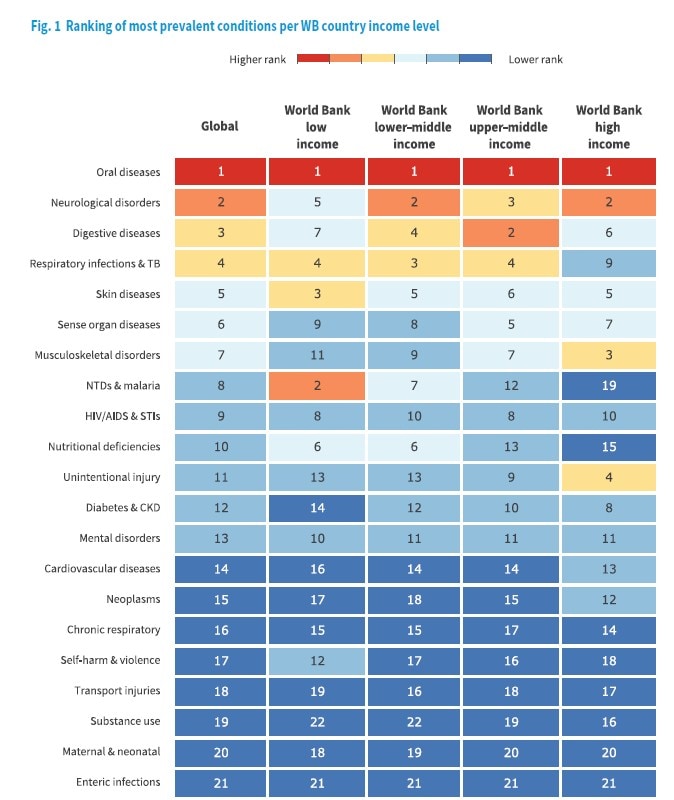
Ranking of most prevalent conditions per World Bank country income level.
Work in Timor and Fiji
Poor oral health is a complex and intractable problem. It fundamentally shapes the qualities of everyday life, the capacity for basic needs to be met, and it introduces mortality amongst groups of otherwise healthy individuals. It is not a matter of having clean teeth or teaching people to clean their teeth regularly to improve oral health; it is a fundamentally social, cultural and economic formation, manifest in the undulations of class, ethnicity, geography, gender and many more aspects of biography.
In a current project led by Professor Michele Ford and Professor Woosung Sohn, the team depart from the understanding that oral ill-health is not simply the result of ‘poor choices’, ‘low education’ or ‘irresponsible behaviour’ – or even a lack of access to oral health professionals or nutritious food. It is a product of a complex constellation of economic, social and cultural factors that shape the behaviour and experiences of individuals and their communities.
Oral health reflects exposure to markets, access to formalised education, parenting modelling and cultural standards. Patterns in oral health are intergenerationally mediated; situated in (local) parenting customs, which are situated within broader societal and cultural customs. The result is many local habits are in place before we have agency over our oral health practices.
Given these dynamics, it is perhaps unsurprising that medically driven models have failed to address the problem.
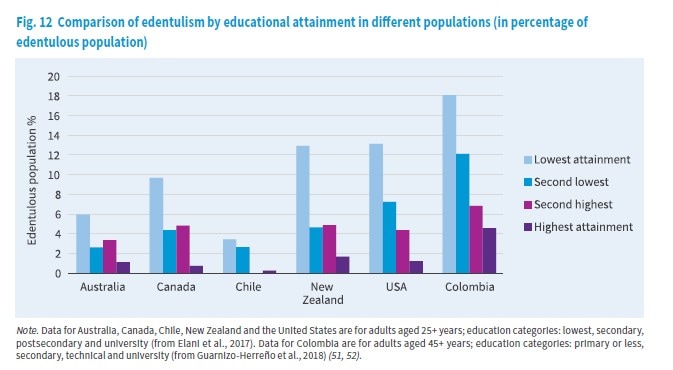
Comparison of edentualism by education attainment in different populations (in percentage of edentulous population).
Comparison of edentualism by education attainment in different populations (in percentage of edentulous population). (Click to enlarge.)
With Professor Woosung Sohn as the oral health lead, the team aim to identify these factors by mapping the political economy of oral health in Timor-Leste, focusing on the factors that shape the context in which individuals and communities make their choices about consumption and preventative practices, as well as treatment. They will examine the oral health beliefs that underpin the choices that individuals, families and communities make about consumption patterns and oral health practices.
In Fiji, Dr Christian and Professor Woosung Sohn are working with Fiji National University’s Dental School to explore a collaboration on population oral health education and research.
Related articles
Supporting better health for First Nations communities

