BJSM Editorials
In a series of three editorials published in the British Journal of Sports Medicine, the international team of scientists discuss issues facing the wearables field including lack of standardisation of devices and data, disconnects between research and industry and the impact of inequality in ownership.
Currently around a third of UK adults own a smartwatch or fitness tracker. A 2021 Australian-based survey reported 24 percent used fitness trackers and 23 percent used smartwatches.
Some use them to track their steps, others their sleep, but few understand the potential of these devices to transform our understanding of how everyday activity influences health.
“If you ask someone how much exercise they did today they will answer none if they missed the gym at lunchtime, but their fitness tracker may tell a very different story,” said Emmanuel Stamatakis, Professor of Physical Activity, Lifestyle and Population Health at the University of Sydney’s Charles Perkins Centre, who co-led the editorial series.
“The device will pick up the short bursts of physical activity, for example when they run for the train or powerwalk to work.
“The use of wearable devices in research, paired with rapidly developing AI, allows us to unlock how these micropatterns of daily activity relate to a person’s risk of premature death, cardiovascular disease and even cancer.
“It’s an exciting time to be working in this area of research.”
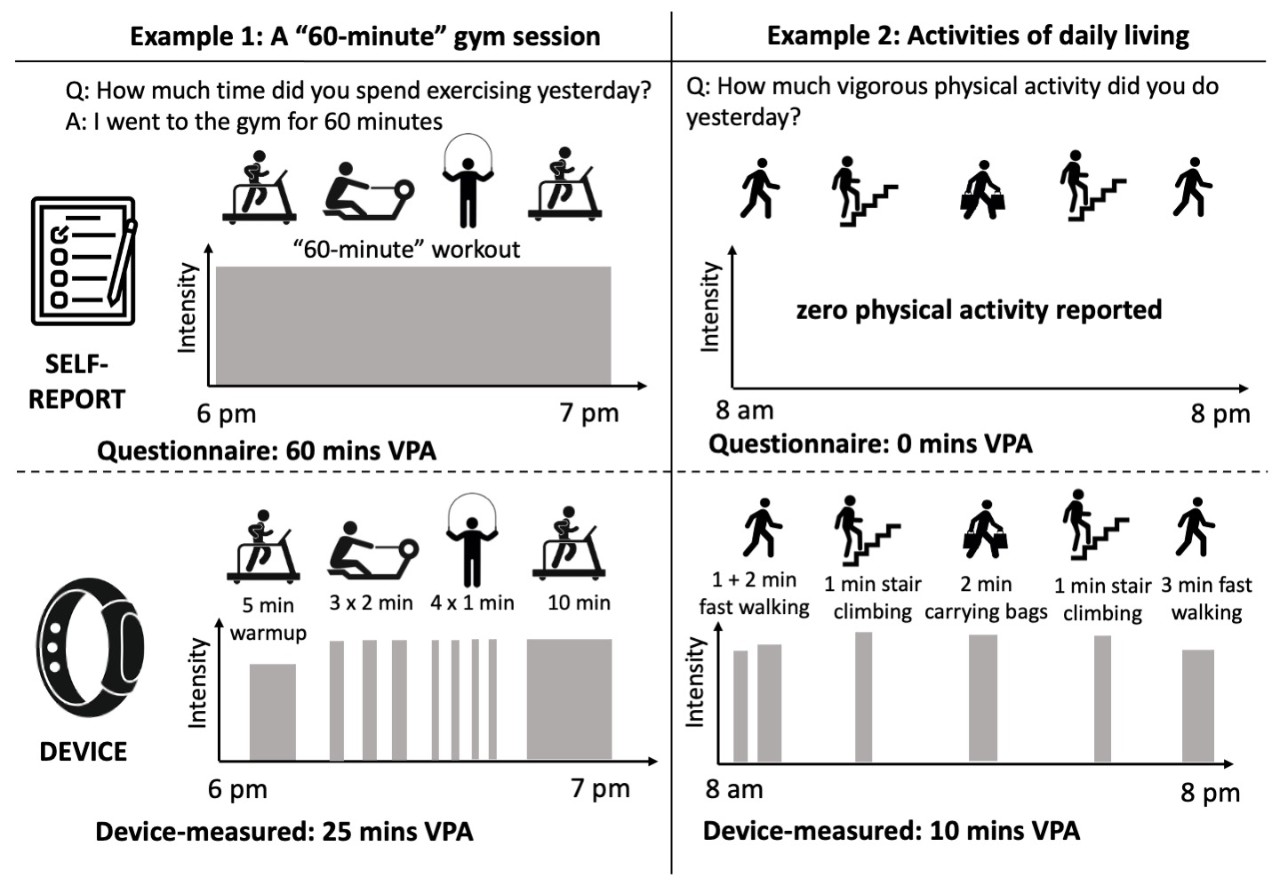
Physical activity captured by self-report questionnaire (top panels) versus wearable device (bottom panels) in two different scenarios. Source: Figure 1 in Gill JMR, et al. Br J Sports Med August 2023
“We now understand that the relationship between physical activity and health is much stronger than previous studies based on self-reported data suggested,” adds series co-lead Jason Gill, Professor of Cardiometabolic Health at the University of Glasgow.
“It is important to harness the capabilities of wearables as research tools because they have so much potential to inform guidelines for how much and what types of activity we recommend people undertake to improve their health, as well as providing new approaches to help support to people to become more active.”
But the field doesn’t come without its challenges – all exacerbated by the pace of this technology.
“The research cycle can be slow but that’s not an option here. We have to adapt and move quickly if we are going to make the most of the opportunities wearables present - or be prepared to miss the train, ” said Professor Stamatakis, who is also launching the Mackenzie Wearables Research Hub at the Charles Perkins Centre, University of Sydney, Australia this week.
Generously funded by the Jenny Mackenzie Bequest to the Charles Perkins Centre, the Hub aims to optimise wearables-related research methods, to be a bridge between academia and industry and to accelerate the evolution of research-grade wearable hardware.
Already researchers at the University of Sydney are exploring innovative uses of trackers to understand whether physical activity is incidental or leisure-time exercise and partnering with dieticians to use wearables to accurately observe daily eating patterns.
While individuals tracking their own activity use consumer devices like Fitbit or Garmin, most research studies use research-grade accelerometers due to their consistency and scientifically documented properties. Consumer devices operate on proprietary algorithms that are “black boxes” to scientists. There is also a lot of variation between brands and models, frequent model updates, and strict corporate rules around data ownership and privacy.
The researchers suggest industry and academics will need to work together a lot more closely on consistency around capabilities and activity metrics for consumer wearables to become a valid source for research measurement and monitoring of health behaviours at a population level.
“There is immense potential for data from wearable devices to inform clinical decisions about risk, diagnosis and treatment. This is particularly relevant in cardiology because low physical activity increases risk of many heart diseases, while once disease develops it reduces the ability to be active,” said Professor Tim Chico, from the University of Sheffield, lead author on the editorial on device-based measurement of physical activity in cardiovascular healthcare.
However, despite the hundreds of device models currently in use, very few are approved for clinical use by regulators. The authors write that incentives for manufacturers to obtain such expensive approvals are small compared with direct sales as “well-being tools.”
The range of measures and accuracy of devices is also a concern in this context, as is the need to have data available to health professionals at the point of decision-making. This raises other questions about the transfer of data from individuals’ devices to their medical records, security and privacy protection, as well as IT capabilities – particularly in less developed nations.
Regulatory frameworks have not adapted to the very fast pace of wearables and big data evolution.
Ninety-three percent of people in the UK and around 90 percent of Australians own a smartphone capable of counting steps which presents huge opportunities for public health.
Tracker and smartwatch use is also growing exponentially, however, there are distinct socioeconomic inequalities in ownership. This presents a problem for using consumer wearables to support positive behaviour change. While people in lower socioeconomic groups are at higher risk of lifestyle-related chronic disease and may have the most to gain from such behaviour change, the purchase of these devices could be well outside their means.
The researchers suggest that none of these challenges are insurmountable.
They argue that better integration of wearables in randomised controlled clinical trials and cohort studies is drastically needed. They suggest that regulators consider the approval of select devices as add-ons to standard care and that industry and academia work more closely together to maximise the potential of wearables for chronic disease diagnosis, prevention, and treatment – with the ultimate goal of a happier and healthier population.
Declaration: Professor Gill is Deputy Director for Physical Activity and Population Health at BJSM. Professor Stamatakis is funded by an Australian Health and Medical Research Council (NHMRC) Investigator Grant. Professor Chico is supported by the NIHR Sheffield Biomedical Research Centre. View the editorials for details regarding other authors. No funders had any input to the editorials.