Retrospective study

Developing effective protocols to diagnose, monitor and treat eye diseases is an extremely challenging endeavour, and even more so when these conditions are rarely encountered or present unclear symptomalotogies.
Uncertainty arising from asynchronous clinical features as well as potentially unknown contributors to rare eye conditions make it difficult to pin down the exact disease profile, thus leading to lengthy diagnoses and delayed interventions.
This is particularly relevant when conditions presenting with early onset visual decline result in various forms of neurodegeneration, as in the case of CLN3 disease, formerly known as juvenile neuronal ceroid lipofuscinosis (jNCL).
NCLs are a group of autosomal recessive lysosomal storage disorders (LSD) and together are one of the most frequent causes of neurodegenerative disease in children
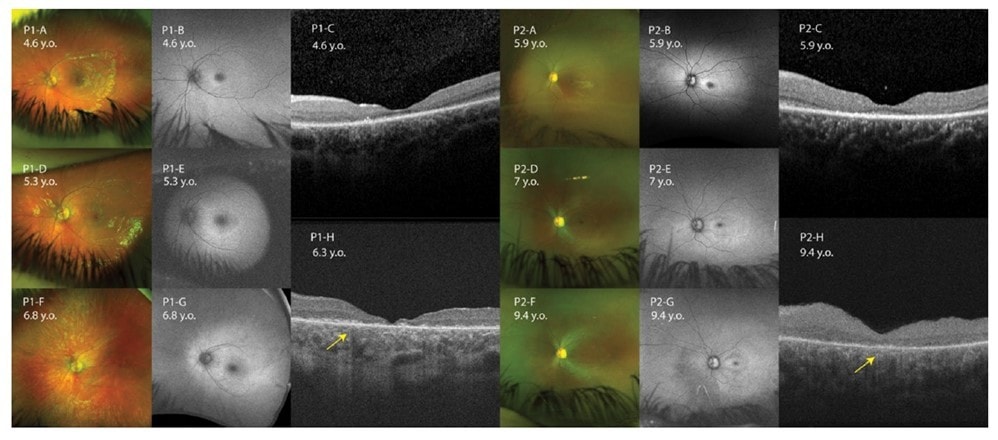
Sourced from Sakti et al. 2023.
As a result of these debilitating conditions, NCL patients generally experience myoclonic seizures, progressive visual deterioration, cognitive dysfunction, motor decline, and premature death.
Early diagnosis of NCLs is therefore vital to ensure clinical intervention at a time when maximal benefit might be achieved.
Under the guidance of Professor John Grigg, Save Sight Institute researchers and clinicians have conducted a retrospective study on young patients affected by CLN3 to help facilitate early recognition via a combination of visual electrophysiology and multimodal imaging.
The clinical features observed in this young cohort of patients were especially informative given that the visual decline in children with CLN3 disease is often more rapid than other early onset maculopathies such as Stargardt disease.
Most importantly, results from this pioneering study point to an electronegative ERG with concurrent bull’s eye maculopathy in young age as reliable biomarkers that should prompt early neurological assessment and genomic investigation for CLN3 gene defects.
Timely recognition of these features will assist in establishing an early diagnosis, thus enabling appropriate therapies, family planning, disease monitoring, and potential enrolment in clinical trials for novel therapies.
As the authors highlight in their publication, monitoring visual function in CLN3 patients becomes increasingly challenging as the neurological deterioration progresses.
Ophthalmologists play an important role in the early detection of this devastating condition. Our work provides guidance for eye care teams.
Therefore, identifying ocular biomarkers and structural parameters that can be consistently recorded in an outpatient setting can largely facilitate the clinical intervention and treatment process.
Given the broad range of eye diseases our SSI clinicians manage on a daily basis, research studies elucidating the signs and symptoms of many such conditions pave the way to the development of appropriate and effective therapies, thus having a positive impact on the life of thousands of people across the globe.